Kampala Emergency Digital Transport System (KEDTS)
New
A free online referral platform in Kampala, Uganda that providers referrals between health facilities and from the community.

As low- and middle-income countries transition from paper to digital systems, family planning programs can benefit from unprecedented opportunities to improve services. Investments in digital health tools have expanded exponentially, but information on what works—and what does not— remains limited and scattered. As investments have increased, digital applications and data fragmentation have proliferated, but stakeholders are moving towards more coordinated efforts to scale digital health solutions, support countries’ digital health infrastructure, and share evidence-based learnings.
This Digital Health Compendium enables users to explore case studies across a range of digital health technologies used to enhance family planning programs mainly in sub-Saharan Africa, but also in other regions of the world. Digital health applications in family planning programs can be broadly classified as those affecting demand generation, service delivery, supply chain management, and the policy and enabling environment. In many low- and middle-income countries, digital health innovations were adopted earlier in other health sectors, including HIV/AIDS, maternal and child health, and noncommunicable disease prevention and response. As a result, much of the impact evidence is likewise restricted to those sectors. To advance greater adoption of digital technology in family planning programs, more data and information on the challenges, opportunities, scalability, and results are needed. This compendium aims to consolidate emerging information and data on applications of digital technology in family planning programs to inform adoption and scale-up of successful approaches.
All of the case studies were submitted by the implementing organizations and include a description of the digital health intervention, program context, and, if available, important findings and lessons learned through rigorous evaluations or program data. The compendium facilitates a quick search for case studies based on the target user for digital health intervention, building block for the digital health enabling environment, family planning program classification, and country location. The case studies give policy and program decisionmakers insights on real-world applications of digital health, promising practices, challenges, and other lessons that can be applied to current and future programs.
New
A free online referral platform in Kampala, Uganda that providers referrals between health facilities and from the community.

Henry Kaula
Learning and Adaptation Lead
Email
Population Services International Uganda (PSIU)
Ongoing
Population Services International: - Source funding for development of the application.
Outbox(U) limited- Development of the application
Kampala Capital City Authority (KCCA): - Hosting the implementation (pilot) and rollout of the application. Support the testing on and usability, feasibility, and adoption of the application in both public and private health facilities in greater metropolitan Kampala.
USAID
Kampala, Uganda
Client, Health Care Provider, Health System Manager
Services and Applications
Demand Generation, Service Delivery, Supply Chain Management, Policy and Enabling Environment
The Kampala Emergency Digital Transport System innovation was borne out of the United States Agency for International Development (USAID) implementation research project called the Maternal and Newborn health project (MaNe). Formative studies conducted in the project’s first year highlighted various barriers to the uptake and utilization of pre-hospital emergency care within the urban poor population.
1. Very few public ambulances are available to meet the needs of the urban poor. Kampala Capital City Authority (KCCA) has only seven ambulances. The existing private ambulances are not leveraged and not well coordinated in addition to the high costs.
2. Poor real-time coordination and view of ambulances in Kampala city for emergency response for maternal and newborn cases (MNH) and other cases including empty referrals, poor patient preparedness and pre-referral care for referring units, poor anticipation of the referral by the receiving facility, and inability to ascertain outcomes and feedback on the referrals made.
3. Poor documentation of the referrals reduced the opportunity for learning from the referrals made.
The Kampala Emergency Digital Transport System (KEDTS) has been developed to address the above issues through improved coordination of the scarce public ambulance resource, leveraging the private sector, data, and documentation for decision-making, and outcomes of the referred cases.
The Kampala Emergency Digital Transport system is a free online referral platform designed
with support from USAID. The system has two modules: the Interfacility module (facility to facility referrals) and the Community module (Community to facility referrals). The platform has interfaces for the facilities (both referring and referral facilities), an interface at the call and dispatch center through which the coordination of all referrals is done, and the ambulance interface for the ambulance teams. 

Figure 1 Micro Level features of the interfacility module.

Referring facilities have been able to log in and decipher the interventions undertaken for a particular referral. This has provided opportunities for learning and decision-making for similar cases.
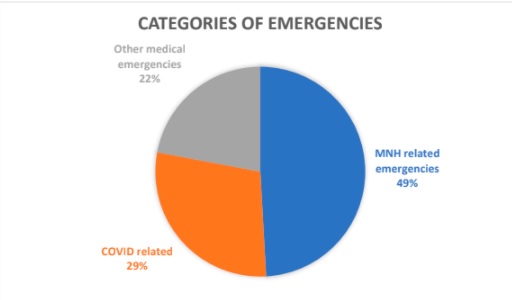
The Kampala Emergency Digital Transport System has been utilized to coordinate and streamline maternal and newborn emergencies, COVID-19 referrals, and other medical emergencies within the Kampala Metropolitan area. Private and public facilities have been oriented on this system and continue with enthusiasm to create both micro and macro networks for referral.
Having all this information on one system has allowed for a central repository of all referral data within Kampala. This allows for real-time reporting, data analysis, evidence generation, and informed decision-making at the management level. The system is currently being linked to the Ministry of Health through the DHIS2 portal and there is potential for integration with the existing Uganda Open Electronic Medical Records to further merge patient records.