Delivering Innovation in Self Care (DISC) Project: Consumer Digital Companion
New
An automated virtual assistant/chatbot that supports clients with information on contraception methods including self-injection.

As low- and middle-income countries transition from paper to digital systems, family planning programs can benefit from unprecedented opportunities to improve services. Investments in digital health tools have expanded exponentially, but information on what works—and what does not— remains limited and scattered. As investments have increased, digital applications and data fragmentation have proliferated, but stakeholders are moving towards more coordinated efforts to scale digital health solutions, support countries’ digital health infrastructure, and share evidence-based learnings.
This Digital Health Compendium enables users to explore case studies across a range of digital health technologies used to enhance family planning programs mainly in sub-Saharan Africa, but also in other regions of the world. Digital health applications in family planning programs can be broadly classified as those affecting demand generation, service delivery, supply chain management, and the policy and enabling environment. In many low- and middle-income countries, digital health innovations were adopted earlier in other health sectors, including HIV/AIDS, maternal and child health, and noncommunicable disease prevention and response. As a result, much of the impact evidence is likewise restricted to those sectors. To advance greater adoption of digital technology in family planning programs, more data and information on the challenges, opportunities, scalability, and results are needed. This compendium aims to consolidate emerging information and data on applications of digital technology in family planning programs to inform adoption and scale-up of successful approaches.
All of the case studies were submitted by the implementing organizations and include a description of the digital health intervention, program context, and, if available, important findings and lessons learned through rigorous evaluations or program data. The compendium facilitates a quick search for case studies based on the target user for digital health intervention, building block for the digital health enabling environment, family planning program classification, and country location. The case studies give policy and program decisionmakers insights on real-world applications of digital health, promising practices, challenges, and other lessons that can be applied to current and future programs.
New
An automated virtual assistant/chatbot that supports clients with information on contraception methods including self-injection.

Betty Nakabiito Musoke
Country Digital Manager
Email
Population Services International - Uganda
Ongoing
Population Services International (PSI)
Society for Family Health (SFH) Nigeria
Children's Investment Fund Foundation (CIFF)
Betty Nakabiito Musoke
Country Digital Manager
Uganda Nigeria
Client
Services and Applications
Service Delivery
Population Services International – Uganda (PSIU)’s digital health strategy aims at leveraging digital technologies and partnerships for improved consumer health and well-being.
The Delivering Innovation In Self Care (DISC) project was launched in January 2020 and runs until December 2024. The project is implemented in Uganda and Nigeria by Population Services International (PSI), Population Services International – Uganda (PSIU), and the Society for Family Health (SFH). The five-year project is funded by the Children’s Investment Fund Foundation and supports women’s knowledge and demand for self-care, beginning with the subcutaneous depot medroxyprogesterone (DMPA-SC) for self-injection. This intervention paves a pathway to self-care as a viable cornerstone of sexual and reproductive health (SRH) and places more power in the hands of women.
The DISC project aims to demonstrate that self-care, beginning with contraceptive self-injection (SI), is a viable cornerstone of SRH. Based on the findings from a study conducted by PSIU, the average woman targeted by the intervention does not see contraception as relevant or valuable in achieving her life goals. If she does know about contraceptive methods, she is unlikely to know about self-injection. She is aware of the stigma and risk involved in seeking SRH information and services. She sees her decision to self-inject as risky, so she desires discretion and convenience among other factors. Armed with these findings, and after a series of testing phases, the PSI team set out to implement the digital companion as a private and confidential source of information to help the woman decide and choose self-injection as a method of contraception.
Launched by the DISC project in Uganda and Nigeria in January 2021, the digital companion is an automated virtual assistant/chatbot hosted on three channels (WhatsApp, Facebook Messenger, and the chatbot embedded in the website) that supports clients with information on contraception methods including self-injection.
The DISC project mainly targets urban youth (18 – 24 years) with disposable income. Also, urban and peri-urban mothers of at least 20 years with access to digital channels and disposable income.
DISC’s inception period comprised formative research, insight generation, and evidence-based prototyping to develop an intervention to catalyze providers’ and consumers’ interest in and demand for DMPA-SC and contraceptive self-care more broadly.
In early 2021, reflecting on insights gleaned from the inception period results, DISC and its stakeholders narrowed their scope to focus more explicitly on fostering women’s knowledge and demand for Self-Injection (SI). The Digital Companion is promoted through ‘’the discover your power’’ multi-channel campaigns that are run on social media platforms (Facebook, Twitter, and Instagram).
DISC’s core focus areas include developing and implementing proven demand generation interventions for SI, innovating to bridge critical gaps in the consumers’ use journey, and knowledge translation to enable other key market actors to optimize demand generation and SI support services. The digital companion was developed as part of this consumer ecosystem.
The digital companion enables clients to view videos or illustrations on self-injection.
Additionally, it assists clients in finding a health facility through a geo-locator that provides useful information like operating hours, services provided, physical location, and contact details. The ‘help’ function supports clients who require more information and wish to interact and have their queries answered by a human.
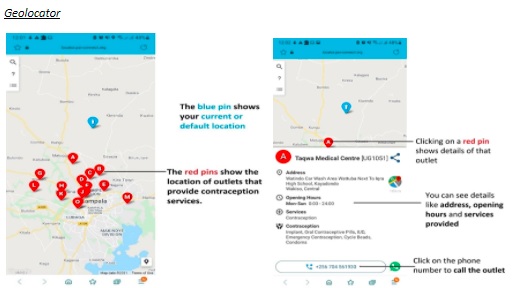
Should a woman choose to take up a contraception method, the digital companion can schedule her follow-up visit and send a reminder a couple of days before the visit to help her not miss her clinic appointments.
The DISC digital companion dashboard demonstrates performance against key metrics, organized along the consumer journey. This helps us understand where we need to focus or optimize our interventions to make the client’s SI journey as frictionless as possible.
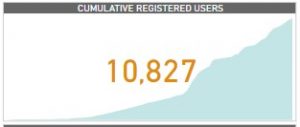
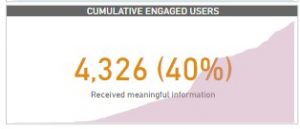
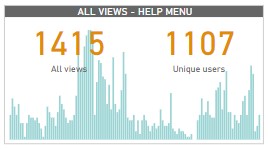
By mid-September 2021, there are nearly 10.78K unique users, with 40 percent meaningfully engaging with the content. Meaningful engagement entails signposting the majority of the users to have read most of the content appropriately to learn more about self-injection contraception.
Figure 1: Cumulative and Engaged users of the digital companion.
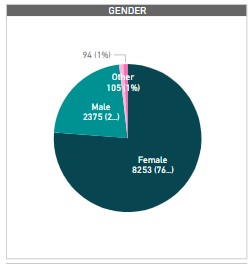
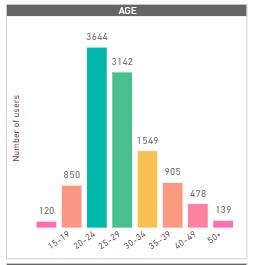
There are more urban female users aged 20 – 34 interacting with the digital companion implying we are reaching and serving our target audience.
Figure 2: Categorization of users by gender and sex
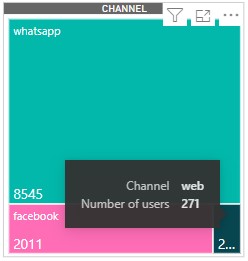
The majority of women in urban and peri-urban areas who own a smartphone use WhatsApp and Facebook as the preferred channels of interaction with the companion with WhatsApp taking the largest share at 91 percent.
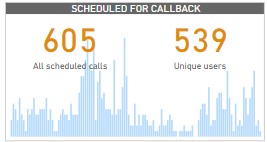
Figure 3: Categorization of beneficiaries by the platform used So far, there are 1,103 unique users with 604 call requests registered on the digital companion call back feature. Out of these, 508 cases were addressed successfully, phone numbers of the remaining 16 percent of the requests could either not be reached or registered as wrong numbers.
Regarding the reasons for the call, 53 percent of the calls sought information on family planning, 41 percent were generally on SRH, and a few (3 percent) requested information on general health issues. The rest were non-health requests. Specific requests on self-injection were on how and where to locate a facility for uptake (42 percent) and side effects of using DMPA-SC (48 percent). Also, 10 percent wanted to know how DMPA-SC works, the site of the injection, and the duration of action. (Figure 4)
CONCLUSION:
DISC will continue to innovate to close the gap between clicks/registered users and increase engagement on the companion. DISC has outlined a set of optimizations that can be made to the user flow to reduce the steps to reaching the information users want, for example, simplifying the menu, shorter registration process, etc. Consideration for a future solution could be for a more dynamic, AI-driven chatbot covering a range of SRH self-care products that deliver on the consumer experience. Based on the increasing number of users who register and interact with the content therein, the digital companion has the potential to be scaled up, shared, and disseminated beyond PSI as a tried and tested digital solution for adoption by both national and private sector partners for SRH information dissemination.
In Uganda and SFH in Nigeria, PSI has made great strides towards leveraging digital technology to improve the client’s access to quality information, products, and services for better health outcomes. The implementation of digital tools like the digital companion has enabled PSIU to serve the consumer better using digital innovations.
DISC Project, (2021). ‘Highlights: Insights synthesis, Insights gained through Evidence-based design’, 26 Pages. https://www.psi.org/wp-content/uploads/2021/08/DISC-Insights-Synthesis-Report.pdf