Digital Training Approaches for Family Planning Clients and Health Workers
Connecting solutions for education and empowerment
As low- and middle-income countries transition from paper to digital systems, family planning programs can benefit from unprecedented opportunities to improve services. Investments in digital health tools have expanded exponentially, but information on what works—and what does not— remains limited and scattered. As investments have increased, digital applications and data fragmentation have proliferated, but stakeholders are moving towards more coordinated efforts to scale digital health solutions, support countries’ digital health infrastructure, and share evidence-based learnings.
This Digital Health Compendium enables users to explore case studies across a range of digital health technologies used to enhance family planning programs mainly in sub-Saharan Africa, but also in other regions of the world. Digital health applications in family planning programs can be broadly classified as those affecting demand generation, service delivery, supply chain management, and the policy and enabling environment. In many low- and middle-income countries, digital health innovations were adopted earlier in other health sectors, including HIV/AIDS, maternal and child health, and noncommunicable disease prevention and response. As a result, much of the impact evidence is likewise restricted to those sectors. To advance greater adoption of digital technology in family planning programs, more data and information on the challenges, opportunities, scalability, and results are needed. This compendium aims to consolidate emerging information and data on applications of digital technology in family planning programs to inform adoption and scale-up of successful approaches.
All of the case studies were submitted by the implementing organizations and include a description of the digital health intervention, program context, and, if available, important findings and lessons learned through rigorous evaluations or program data. The compendium facilitates a quick search for case studies based on the target user for digital health intervention, building block for the digital health enabling environment, family planning program classification, and country location. The case studies give policy and program decisionmakers insights on real-world applications of digital health, promising practices, challenges, and other lessons that can be applied to current and future programs.
Connecting solutions for education and empowerment

Beth Balderston
Communications Officer
PATH
Email
PATH (lead)
Ministries of Health in Senegal and Uganda (collaborators, host countries)
John Snow, Inc. (collaborator)
Bill & Melinda Gates Foundation
Children’s Investment Fund Foundation
2018 - present
Uganda, Senegal
Client, Health Care Provider
Workforce
Service Delivery
Training and supervising health workers is one of the biggest challenges and cost drivers when introducing and bringing to scale a new contraceptive method or service delivery innovation.
Traditional in-person trainings bring together health workers for multi-day events, which typically include both classroom and practical hands-on training. This approach can require thousands of dollars for per diem, travel, materials, facilitation fees, and room rentals.
Moreover, off-site trainings can leave facilities short-staffed, resulting in delays in service delivery while providers are in training. In-country scale-up plans for the injectable contraceptive subcutaneous DMPA (DMPA-SC), training is the highest-cost activity—often representing 50 percent or more of costs.
Contraceptive self-injection has received strong endorsement from the World Health Organization as a self-care intervention that can both alleviate burdens on health systems and empower women to manage their own health. Yet, while having clients self-inject DMPA-SC is an effective task-shifting strategy in the long run, health workers must find time up front in their busy schedule to counsel and coach clients who are new to the practice.
In response to the pressing need for more affordable training approaches that maintain quality of care, PATH has developed digital training resources for both DMPA-SC self-injection clients and health workers who provide family planning and are learning to offer DMPA-SC as an option amid a wide range of contraceptive methods in private, public, or community-based sectors.
PATH, in collaboration with John Snow, Inc., produced short five- to seven-minute training videos for both self-injection clients and health workers learning to administer DMPA-SC. Available in English and French, these videos are intended to complement any training approach. The script and video files are also available for translation or adaptation to fit specific program contexts. To date, the videos have been used and adapted in several countries, including Mauritania, Nigeria, Senegal, Uganda, and Zambia.
In addition to the videos, PATH has developed an eLearning course designed for health workers who are learning to offer DMPA-SC. The course is based on PATH’s original classroom-based curriculum that has been used for many years to train health workers with diverse levels of expertise. The online course is available in English and French and can be taken on computer, tablet, or mobile phone with internet access. Participants can either take the full 10 lessons or the individual lesson on counseling clients on self-injection. Interactive exercises, resources, and job aids are included throughout the course to help learners engage with the information. Participants are required to pass quizzes on individual lessons and a final quiz to earn the course certificate of completion.
Both the training videos and eLearning course are designed for clients and health workers across sectors, including public facilities, private clinics, pharmacies, or drug shops. They are also intended for use in the context of an in-person orientation, such as a counseling session for clients or a hands-on practicum for health workers before they are authorized to administer injections to clients.
While digital training approaches have great potential to facilitate DMPA-SC training worldwide, limited information is available on their implementation in low-resource settings. To learn more about whether and how these approaches could be effective, we conducted an evaluation of clients learning to self-inject using the video in Uganda. In Uganda and Senegal, we are currently conducting evaluations of our eLearning course.
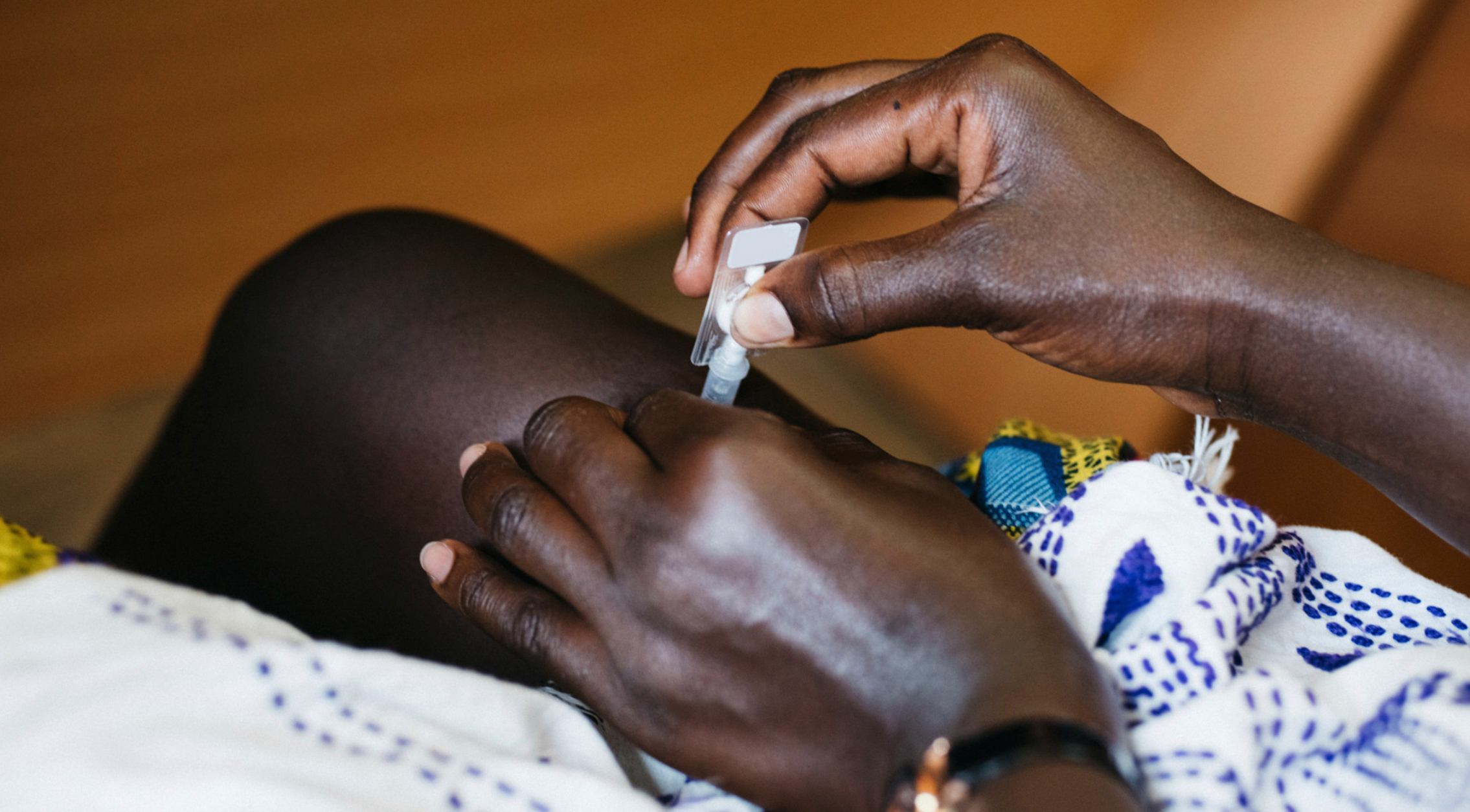
The self-training study evaluated client’s self-injection competency after watching the five-minute video compared to those who learned with a two-page printed self-injection job aid We randomly assigned either the video or job aid to 200 women who were clients in public clinics (n=101), private clinics (n=38), pharmacies (n=24), or drug shops (n=37) across five districts in Uganda. After self-training, clients demonstrated how to inject on a model; as this was a proof of concept, no actual self-injecting took place.

Overall, clients found the video easier to follow when accompanied with the printed job aid. In both the video and job aid groups, over half of clients reported feeling “very prepared” to demonstrate the injection, were generally satisfied with self-training (video clients more so), and said they would recommend it to their friends.[5]

Across sectors, clients who self-trained with the video had higher competence (71 percent) than those who used the job aid (36 percent). In the public sector, clients who watched the video were more likely to correctly calculate reinjection dates. Private sector clients had higher competency than public sector clients whether they self-trained with the job aid or the video.

After an initial round of pretesting and revisions to the eLearning course based on health worker input, we are evaluating the DMPA-SC eLearning course in select parts of Uganda and Senegal in collaboration with the ministries of health. This evaluation aims to determine whether the approach is effective, feasible, and cost-efficient; for whom the approach works well and for whom it does not; and what the facilitators and barriers are for successful application of eLearning as a family planning training approach. The evaluation is currently underway in Uganda, with results expected mid-2020. The evaluation in Senegal is anticipated to begin in mid-2020.
Our experience introducing digital training has shown great potential to help reduce the costs, time, and inconvenience associated with traditional training approaches in family planning programs. To date, both clients and health workers have expressed satisfaction with these interventions, and there is growing evidence indicating their effectiveness.
Before introducing any digital training innovation, a deep understanding of the anticipated context of use is crucial. Accounting for key factors—such as access to devices, connectivity, and users’ familiarity with digital platforms—as early as possible during the development process is more likely to lead to success.